Category Archives: Bone and Nerves
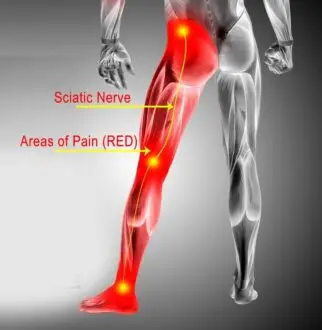
How to Treat Sciatica and Nerve- Effective Sciatica Treatment and Nerve Pain Relief
How to Treat Sciatica and Nerve Pain If you’re struggling with sciatica and nerve pain, [...]
14
Jun
Jun
Numbness relief/Effect and Solution for Nerve Numbnes2
Numbness in hands and feet How to Treat Numbness: Effective Solutions for Nerve Numbness and [...]
29
May
May
How to maintain Healthy bones 2
Balanced Diet for Bone Health Healthy Bones -Maintaining robust bone health necessitates a balanced diet [...]
Bone Health| Bad Health Challenges Of The Bone4
Common Bone Disorders The phrase “Common Bone Disorders” encompasses a variety of conditions that can [...]
14
Oct
Oct
What is Bone Health
Preserving the health of your bones is vital for your overall wellness and life quality. [...]